Heart failure phenotypes span reduced ejection fraction (HFrEF), mildly reduced (HFmrEF), and preserved ejection fraction (HFpEF), and each group needs tailored therapy. The evolution to quadruple GDMT marks a clear shift away from traditional dual therapy and closes many of the outcome gaps seen with older regimens. Real-world implementation still lags guideline recommendations, especially in HFrEF populations. Remote monitoring technologies, particularly CardioMEMS pulmonary artery sensors, extend this pharmacologic foundation by enabling intervention before symptomatic deterioration. These combined advances support operational gains, including a 50% reduction in 30-day readmissions and stronger CPT billing performance for 99454 and 93298. This article first examines the pharmacologic foundation with quadruple GDMT, then shows how remote monitoring and vendor-neutral platforms help teams apply these therapies in real time.
Traditional heart failure management relied on ACE inhibitors and beta-blockers as foundational therapy. This dual approach improved outcomes but left significant residual risk, which modern quadruple GDMT addresses by adding SGLT2 inhibitors, angiotensin receptor-neprilysin inhibitors (ARNI), and mineralocorticoid receptor antagonists (MRA) per ACC/AHA 2024–2026 guidelines. Key shift: these combinations deliver measurable reductions in cardiovascular death or hospitalization for heart failure across phenotypes. The OPTIPHARM-HF registry highlights implementation gaps, with uneven SGLT2 inhibitor use across HFrEF, HFmrEF, and HFpEF. Benefits extend beyond ejection fraction categories and provide consistent outcome improvements across diverse patient populations.
SGLT2 inhibitors now sit at the center of contemporary pharmacologic heart failure treatment, with benefits that do not depend on diabetes status. Dapagliflozin and empagliflozin reduce hospitalization for heart failure across a wide range of kidney function. Key shift: frailty benefits with hazard ratios of 0.71–0.85 show particular value in elderly patients. The RENAL LIFECYCLE Trial continues to evaluate cardioprotective effects in severe chronic kidney disease, dialysis, and transplant populations. These findings expand SGLT2 inhibitor use beyond traditional indications and support their role across the heart failure spectrum. While these pharmacologic advances improve outcomes, their full impact depends on timely detection of decompensation, which modern monitoring technologies now address.
Traditional heart failure monitoring relied on subjective symptoms and periodic clinic visits. Modern outpatient management now incorporates implantable hemodynamic monitors such as CardioMEMS, which measure pulmonary artery pressures every day. Because pressure elevations occur weeks before symptoms develop, clinicians can adjust medications preemptively. This early warning capability explains why Atlantic Health reports significant reductions in heart failure readmissions through real-time pressure monitoring and remote therapeutic adjustments. The battery-free sensor requires about 30 seconds of daily use with a home pillow, which provides objective data and shifts care from reactive to proactive.
Non pharmacological management of heart failure also includes device-based therapies for patients with more advanced disease. Cardiac resynchronization therapy (CRT) improves cardiac performance in patients with left bundle branch block, and CRT improves cardiac performance in LBBB patients who meet guideline criteria. Next-generation left ventricular assist devices (LVADs) such as HeartMate 3 support both bridge-to-transplant and destination therapy strategies. Implantable cardioverter-defibrillators (ICDs) reduce the risk of sudden cardiac death in high-risk cohorts. Expanded use of hepatitis C–positive donors has also increased heart transplant availability. These interventions reduce readmissions and improve quality of life for patients with advanced heart failure phenotypes.
AI-enabled remote monitoring now supports earlier detection of worsening heart failure and more precise therapy adjustments. AI integration enhances echocardiography, MRI, and CT scans by delivering faster, more accurate assessments and reducing human error. HeartLogic multisensor algorithms combine heart sounds, thoracic impedance, respiratory rate, and activity levels to flag early signs of decompensation. Ongoing studies evaluate HeartLogic-guided remote management for reducing death, unscheduled hospitalization, and quality-of-life decline. Data fidelity exceeds 99.9% through redundant feeds and computer vision technologies, which supports reliable AI phenotyping at scale. Beyond technological monitoring, comprehensive heart failure care must also address physiologic deficits and lifestyle factors.
Non pharmacological management of heart failure extends beyond devices to include intravenous iron therapy and structured lifestyle programs. Iron deficiency affects up to half of heart failure patients regardless of anemia status, and IV iron supplementation improves exercise capacity and quality of life. Structured exercise programs, including cardiac rehabilitation and yoga, help reverse ventricular stiffness and improve functional capacity. Regenerative medicine approaches such as stem cell therapies and gene editing show early promise for repairing damaged myocardium. These interventions complement pharmacologic therapy and address underlying pathophysiology that medications alone may not fully correct.
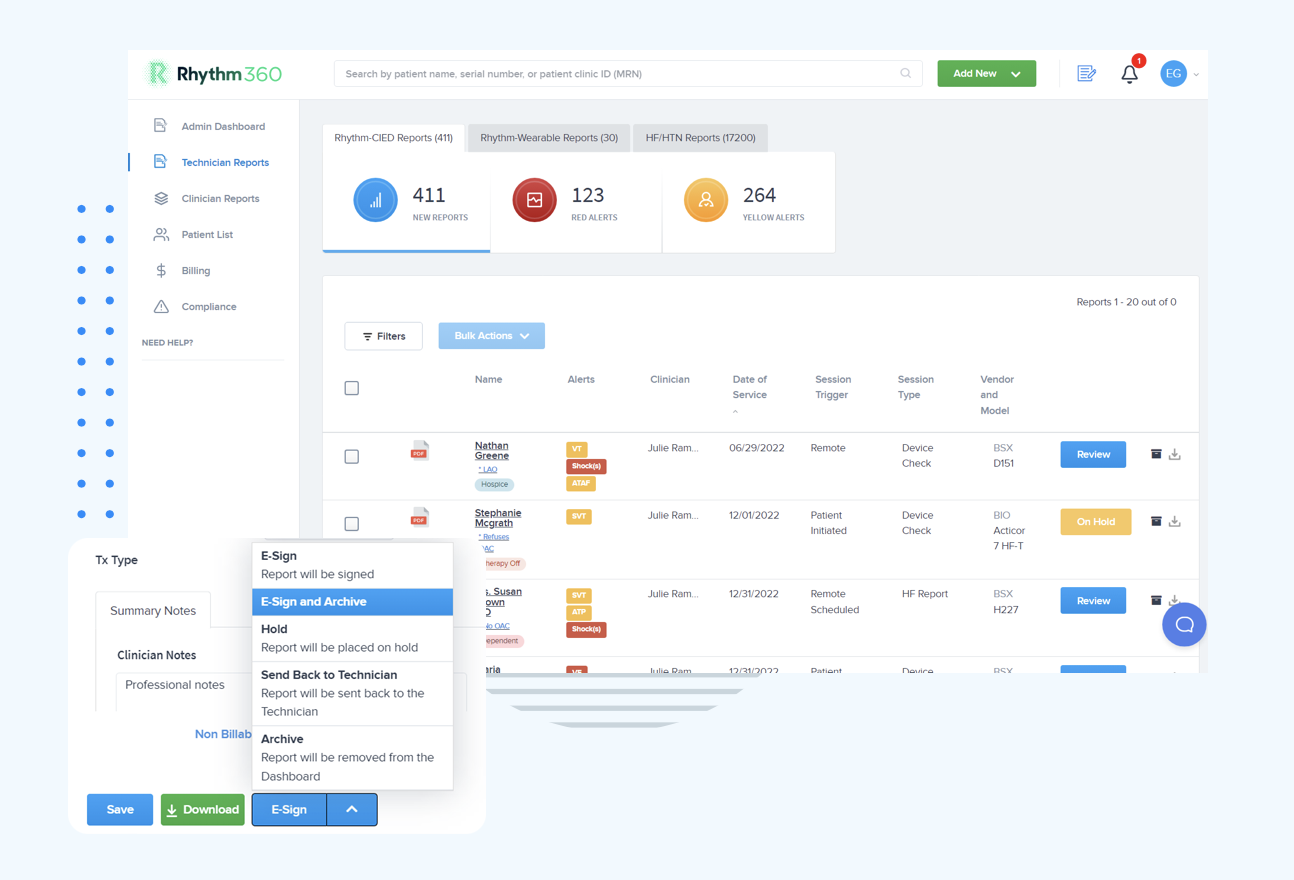
Rhythm360 centralizes modern heart failure management by unifying disparate OEM data streams from Medtronic, Abbott, Boston Scientific, and Biotronik into a single AI-powered platform. Competing solutions such as Paceart or Murj often remain tied to specific vendors, while Rhythm360 delivers vendor-neutral integration with bi-directional EHR connectivity and mobile access. The platform reduces critical alert response times by 80% through intelligent triage and increases practice revenue by 300% through automated CPT capture for 99454 and 93298. Cloud-based architecture with more than 99.9% data fidelity supports reliable monitoring across CIED and physiologic sensors. Transform your heart failure workflows with unified data management, and experience a live Rhythm360 walkthrough to see this model in practice. The table below illustrates how Rhythm360’s unified approach improves three core dimensions of heart failure workflows.
| Aspect | Traditional | Modern (e.g., Rhythm360 RPM) |
|---|---|---|
| Monitoring | Manual OEM portals | Unified AI/RPM (50% readmission cut) |
| Alerts | Fatigue, silos | 80% faster triage |
| Revenue | Leakage | 300% CPT uplift |
The 2026 healthcare landscape shows a clear move from OEM fragmentation toward cloud-based RPM solutions. Cardiology practices face growing pressure from alert fatigue, data silos that block a complete patient view, and revenue leakage due to incomplete CPT documentation. The Cadence nationwide heart failure study reports 18% fewer hospital admissions and $183 per patient per month total cost reduction across 1,786 Medicare fee-for-service patients through reduced inpatient utilization and better guideline-directed therapy. The CMS Ambulatory Specialty Model for heart failure, launching January 2027, will tie reimbursement to quality and cost performance. These forces make efficient RPM platforms essential rather than optional for long-term practice sustainability. To respond effectively, practices need a clear, staged implementation plan.
Successful modern heart failure programs roll out in phases over several days to a few weeks. Initial assessment covers EHR compatibility, current staff workflows, and risk-based stratification of the patient population. Rhythm360 onboarding begins with API integration to connect data sources, which then supports clinical staff training on the unified interface. After staff training, HIPAA-compliant mobile app deployment extends monitoring beyond the clinic and into patients’ homes. These technical foundations enable key milestones such as establishing baseline metrics, customizing alert thresholds for your population, and configuring CPT automation for accurate billing. The build-versus-buy decision usually favors SaaS platforms like Rhythm360 because they provide scalability, regulatory compliance, and ongoing support. Start your implementation blueprint and speak with a Rhythm360 specialist to map your practice’s modernization pathway.
Practices often struggle when they deploy new heart failure tools but keep old data silos in place. Common pitfalls include limited staff training, alert thresholds that do not match the patient mix, and missing baseline metrics that make progress hard to measure. Avoiding these issues directly supports success on core metrics such as hospitalization rates, medication adherence, alert response times, and CPT capture. Success metrics span clinical outcomes, operational efficiency, and financial performance. The following benchmarks, drawn from real-world implementations, show the type of impact practices can expect when they address these pitfalls early.
| Metric | Improvement | Source |
|---|---|---|
| Alert Response | 80% reduction | RhythmScience data |
| Revenue | 300% uplift | RhythmScience cases |
| Readmissions | 18%–50% drop | Cadence/Tenovi |
Remote physiologic monitoring uses CPT codes 99453, 99454, 99457 for the first 20 minutes of interactive clinical staff time reviewing and discussing remote data, and 99458 for each additional 20 minutes. Cardiac device monitoring services use CPT codes 93297, 93299, and G2066. Rhythm360 automates documentation and billing for these codes, which supports compliance and maximizes revenue capture within routine workflows.
Rhythm360’s vendor-neutral architecture ingests CardioMEMS pulmonary artery pressure data alongside other physiologic monitors through standardized APIs and HL7 interfaces. The platform normalizes these disparate data streams into unified patient dashboards that support comprehensive heart failure monitoring across multiple device types. AI-powered algorithms then correlate pressure trends with symptoms and medication changes to provide clear, actionable insights for clinical decision-making.
AI-powered alert triage systems such as Rhythm360 significantly reduce alert fatigue through intelligent filtering and prioritization. Machine learning models analyze historical patterns, patient-specific baselines, and clinical context to separate actionable alerts from routine transmissions. This approach achieves an 80% reduction in non-critical notifications while ensuring urgent events receive immediate attention, which improves clinician efficiency and patient safety.
HFpEF management now includes SGLT2 inhibitors approved for heart failure regardless of diabetes status. These medications reduce hospitalization for heart failure by about 25% across ejection fraction categories, with particular benefits in elderly and frail patients. Quadruple GDMT principles increasingly extend to HFpEF, combining SGLT2 inhibitors with traditional neurohormonal blockade to support broader disease modification.
The Rhythm360 demonstration provides a guided platform walkthrough, an EHR integration review, and a customized workflow analysis for your practice. Technical implementation usually takes several days to a few weeks and includes API setup, staff training modules, and patient onboarding protocols. The demo also covers revenue strategies, alert configuration options, and mobile app capabilities so your team can plan for smooth adoption and rapid value realization.
The shift from traditional reactive heart failure management to proactive, connected care improves outcomes and strengthens practice finances. RPM platforms such as Rhythm360 unify fragmented workflows, shorten response times, and support revenue growth through automated compliance. Take the next step and request a personalized Rhythm360 consultation to modernize your 2026 heart failure management program.


