Multiple device manufacturer silos create transcription errors and missed critical alerts including atrial fibrillation, ventricular tachycardia, and device malfunctions. These data fragmentation issues compound when combined with manual workflows, which struggle to track activity across disconnected systems. The result is missed billable remote monitoring events and lost revenue for undocumented RPM services (99453, 99454, 99457).
Nearly 15–20% of medical claims are denied on first submission, and cardiology practices often see even higher rates due to coding mismatches and documentation gaps. Common cardiology denials stem from unspecified ICD-10 codes, incorrect diagnosis-to-procedure pairing, and missing modifiers, which directly erode margins.
The 2026 updates introduce shorter monitoring windows and stricter device matching requirements, which increase compliance risk for teams using outdated tools. Legacy systems like Paceart lack cloud functionality and AI-powered automation needed for modern telemetry workflows. Practices that continue relying on these systems face ongoing revenue leakage, higher administrative burden, and greater exposure to audit findings.
The following seven strategies form a connected playbook. They start with getting 2026 codes right, then address device-charge matching, denial prevention, KPI visibility, data unification, workflow automation, and finally ROI measurement. Together they create a closed-loop revenue cycle for cardiac telemetry instead of isolated fixes.
Accurate use of new CPT codes anchors every other revenue improvement. CMS’s 2026 Physician Fee Schedule introduces CPT 99445 for 2–15 day monitoring at approximately $47 reimbursement, while existing CPT 99454 covers 16–30 days at approximately $47. The table below summarizes the primary RPM codes and shows how monitoring duration and clinical time drive code selection.
| CPT Code | Description | Duration | 2026 Reimbursement |
|---|---|---|---|
| 99445 | Remote monitoring, device supply | 2–15 days | ~$47 |
| 99454 | Remote monitoring, device supply | 16–30 days | ~$47 |
| 99457 | Treatment management services | First 20 minutes | ~$52 |
Rhythm360 automatically selects the correct CPT code based on actual monitoring duration and documented clinical interactions. Teams then confirm that device data collection periods match billed codes, which prevents denials tied to duration mismatches.
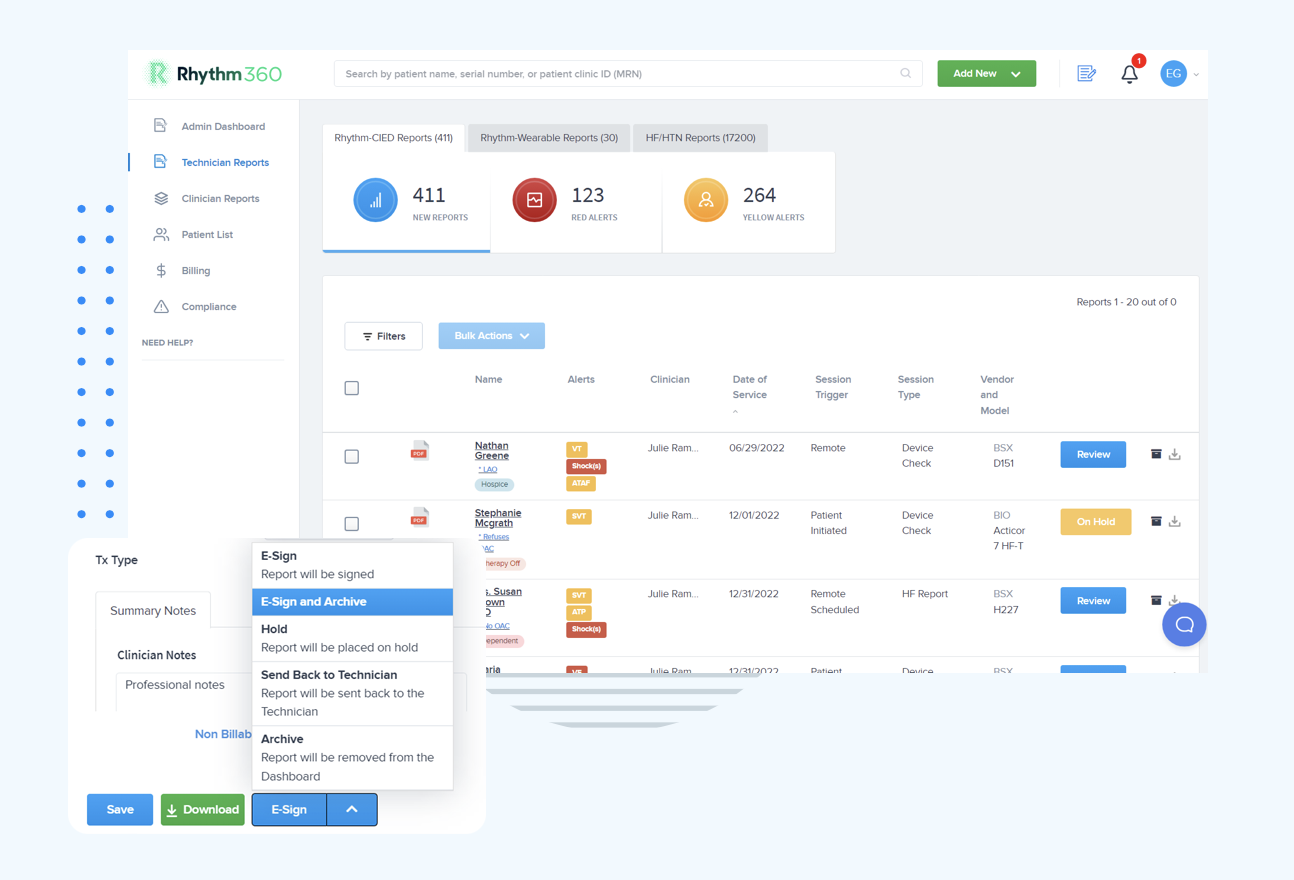
CMS 2026 RPM compliance requires precise documentation of data days and device-supply matching. Workflows that automatically correlate device transmissions with billing periods ensure every eligible day appears in your claims. This alignment protects revenue and supports audit readiness.
Checklists operationalize these workflows for front-line staff. Teams verify transmission dates, patient compliance, and clinical interactions before each claim submission so nothing falls through the cracks. Rhythm360’s vendor-neutral platform automates this correlation and verification by unifying data from major OEMs into one view, which removes the manual matching burden from staff.
Systematic focus on top denial drivers produces the largest near-term revenue lift. Common cardiology denials include unspecified ICD-10 codes, incorrect modifier usage, and insufficient medical necessity documentation. Patient demographic errors and insurance eligibility failures also trigger frequent rejections.
Pre-submission audits address these issues before claims reach payers. Teams check diagnosis-to-procedure alignment, modifier accuracy, and documentation completeness for each encounter. CodaMetrix’s CMX CARE™ reduces coding-related claim denials by up to 60%, which illustrates the impact of automation in this area.
Rhythm360’s AI automation delivers the 80% denial reduction highlighted earlier through three mechanisms. It validates coding choices against payer rules, performs real-time eligibility verification, and confirms documentation completeness for billed services. Together these checks remove the most common denial causes and stabilize cash flow.
Once denial reduction measures are in place, leadership needs visibility into whether they work. Monitoring key performance indicators reveals where revenue cycle gaps remain and which interventions deliver results. Industry benchmarks include denial rates below 5%, days in A/R under 40, and clean claim rates of 95% or higher.
Teams track denial rates by denial code, average collection time, and revenue per patient to pinpoint friction points. First-pass resolution rates and appeal success percentages show how well front-end and back-end processes perform. Rhythm360’s dashboard provides real-time KPI monitoring and alerts leaders when performance drifts from targets, so they can intervene quickly. See Rhythm360’s revenue analytics to understand how this visibility could support your team.
Fragmented device manufacturer portals create heavy administrative work and inconsistent data. Staff must log into multiple systems, rekey information, and reconcile conflicting records, which increases error rates and slows billing cycles.
The contrast between manual and unified approaches appears across every operational metric.
| Approach | Data Reliability | Administrative Time | Error Rate |
|---|---|---|---|
| Manual OEM portals | Variable | High | Higher |
| Rhythm360 unified platform | >99.9% | Reduced 80% | <5% |
As this comparison shows, Rhythm360’s vendor-neutral platform consolidates CIED and RPM data into a single dashboard instead of separate manufacturer portals. This unified view sharply reduces administrative overhead while improving accuracy, which supports both clinical decisions and billing integrity.
Manual alert management slows teams and hides billable events inside noisy queues. Alert fatigue from non-actionable notifications reduces clinical efficiency and causes missed documentation for services that should generate revenue.
AI-powered alert filtering focuses staff attention on clinically significant events and suppresses low-value noise. AI platforms can reduce manual coding work by up to 70%, which illustrates the scale of effort that automation can remove from teams.
Rhythm360’s intelligent alerting system reduces response times by about 80% while ensuring that billable events are captured and documented. Faster triage improves patient outcomes, and complete documentation supports consistent billing for the work your clinicians already perform.
Clear ROI calculations help leadership prioritize telemetry investments and staffing. Revenue modeling should include gains from reduced denials, faster collections, and expanded monitoring services across cardiac and related programs.
A 100-patient cardiac monitoring program can generate more than $200,000 annually when CPT codes are applied correctly and denials fall. Heart failure and hypertension RPM services add recurring revenue streams on top of core telemetry. The revenue impact can be substantial, with customers achieving the 300% increases mentioned earlier by combining denial reduction, shorter A/R cycles, and broader monitoring enrollment into one coordinated strategy. Request an ROI review to see how these levers apply to your practice.
Rhythm360 delivers measurable improvements over legacy and competitive platforms across speed, accuracy, and revenue. Real-world implementations show an 80% reduction in critical alert response times and the 300% revenue increases referenced earlier, driven by unified data management and AI automation.
Examples include electrophysiology clinics that prevent strokes through faster AFib detection and heart failure programs that reduce hospitalizations through earlier intervention. The platform’s vendor-neutral design and >99.9% data reliability distinguish it from single-OEM solutions that keep data locked in silos.
| Feature | Rhythm360 | Legacy Competitors |
|---|---|---|
| Vendor-neutral platform | Yes | Limited |
| AI denial reduction | 80% improvement | Partial automation |
| EHR integrations | Epic, Cerner, others | Limited options |
Teams can begin optimization with a focused set of actions that address data, coding, and technology.
Onboarding typically takes days to weeks depending on EHR integration complexity, and SaaS pricing scales with practice size and usage. Request an implementation roadmap tailored to your telemetry program.
The seven strategies above create a complete framework for improving cardiac telemetry monitoring revenue and billing in 2026. They move from code mastery and device-charge alignment through AI automation, KPI visibility, data unification, workflow efficiency, and ROI tracking.
Rhythm360’s vendor-neutral platform brings these elements together in one system so teams can unify device data, reduce denials, and capture the full value of their clinical work. Fragmented workflows and manual processes no longer need to limit profitability. See how Rhythm360 can transform your telemetry revenue cycle and support your growth plans.
The 2026 CPT code updates introduce CPT 99445 for remote monitoring device supply covering 2–15 days at approximately $47 reimbursement, which expands billing opportunities for shorter monitoring periods. CPT 99470 covers brief treatment management services for the first 10 minutes at approximately $26. These additions allow practices to bill for intermittent monitoring that previously went unbilled, especially for post-hospitalization cardiac patients and medication titration.
Rhythm360 reduces claim denials by about 80% through AI-powered pre-submission validation that checks diagnosis-procedure alignment, modifier accuracy, and documentation completeness before claims go out. The platform automatically verifies patient eligibility, selects CPT codes based on actual monitoring duration, and maintains audit trails for all clinical interactions. This automation removes common denial causes such as coding errors, missing documentation, and eligibility issues.
Most practices see measurable improvements within 30–60 days of implementation, with full ROI typically achieved within 3–6 months. Reduced denials, faster collections, and expanded billable services combine to create multiple revenue streams. A typical 100-patient cardiac monitoring program can generate more than $200,000 annually through proper optimization, while larger practices often report around 300% revenue growth after comprehensive platform adoption and workflow redesign.
Rhythm360 provides vendor-neutral integration with major cardiac device manufacturers including Medtronic, Boston Scientific, Abbott, Biotronik, and others. The platform uses APIs, HL7, XML parsing, and computer vision to normalize data from these sources into a unified dashboard. This approach removes the need for staff to log into multiple OEM portals and supports >99.9% data reliability through redundant data feeds and AI-powered gap filling.
Rhythm360’s HIPAA-compliant mobile application lets clinicians review transmissions, sign reports, and coordinate care from smartphones, which keeps critical patient data available 24/7. This access reduces response times for urgent alerts such as new-onset AFib or device malfunctions and supports faster interventions. The mobile platform maintains full audit trails and integrates with existing EHR systems so clinicians can continue workflows smoothly whether they are in the office or on call.


