Real-time heart failure management platforms bring data from Medtronic, Abbott, Boston Scientific, Biotronik, and other manufacturers into unified clinical dashboards. These vendor-neutral systems use API connections, HL7 integration, and computer vision to standardize data from pacemakers, ICDs, CardioMEMS sensors, and remote physiological monitoring devices.
The 2026 clinical focus centers on AI reliability and workflow automation that clinicians can trust. AI systems now show strong performance in diagnostic tasks while maintaining >99.9% data transmissibility through redundant feeds that prevent data loss. This technical reliability enables practices to pursue expanded remote patient monitoring billing with confidence, generating substantial revenue through precise CPT code capture for 99454, 93298, and 93299.
Cardiology clinics using these platforms report major operational gains. They see 80% reductions in critical alert response times, removal of multi-portal login requirements, and revenue increases up to 300% through automated billing workflows and lower administrative overhead.
The cardiovascular monitoring ecosystem includes fragmented OEM portals, diverse heart failure sensors, EHR systems, and complex billing rules. This fragmentation creates operational pain points that slow teams down and introduce clinical risk.
Administrative teams struggle with multi-vendor portal management that requires separate logins for each device manufacturer. This fragmentation forces staff to spend hours each day pulling patient data from multiple sources, then manually entering information into EHRs. That manual work often exposes conflicting reports across systems, which require extra reconciliation time. The cumulative effect of these redundant workflows reduces time for patient care and raises operational costs.
Clinicians face overwhelming alert volumes that create dangerous fatigue patterns. Studies indicate that 80–99% of alarms from continuous monitoring systems are false or clinically insignificant. This noise hides critical events such as new-onset atrial fibrillation, ventricular tachycardia, or heart failure decompensation, which can lead to missed interventions and adverse outcomes.
Financial leakage also creates pressure as practices miss billable remote monitoring events. Complex CPT requirements for 93298, 93299, and 99454 often cause lost revenue when documentation lacks clear audit trails or required timing details.
The Hospital Readmissions Reduction Program amplifies these challenges. In FY 2026, HRRP penalties increased, with 8.1% of hospitals facing penalties of 1% or more. Proactive heart failure management now supports both patient safety and financial sustainability.
Modern real-time heart failure monitoring platforms use structured data workflows to turn fragmented information into clear clinical actions. The process starts with automated data ingestion from multiple sources using API connections, HL7 feeds, XML parsing, and computer vision for PDF reports.
AI-powered alert triage serves as the key differentiator that changes daily practice. These systems filter non-actionable notifications and highlight clinically significant events. AI triage in remote patient monitoring platforms reduces false positives and unnecessary clinician alerts. This intelligent filtering lets clinicians focus on patients who need immediate intervention instead of fighting constant alarm fatigue.
The table below shows how data moves through each stage of the monitoring workflow and how each step compounds clinical impact.
| HF Monitoring Workflow | Description | Clinical Impact |
|---|---|---|
| OEM Data → Unified Dashboard | Ingest and normalize CIED and HF data via AI and computer vision | Removes multi-portal logins and centralizes review |
| → Prioritized Alerts | AI triage with mobile notifications via Twilio | Delivers the response time improvements noted above |
| → EHR/Billing Integration | Bi-directional Epic and Cerner connections with automated CPT capture | Enables the revenue optimization described earlier |
Mobile access extends this workflow beyond the clinic. HIPAA-compliant applications support remote report review, alert management, and care coordination from any location. This mobility proves vital for on-call coverage when rapid response to critical arrhythmias or heart failure events can prevent hospitalizations.
Rhythm360 illustrates these capabilities with multi-modality support for CIED and heart failure monitoring, oversight by certified cardiac technicians, and high data reliability through redundant transmission pathways and AI-powered gap filling.
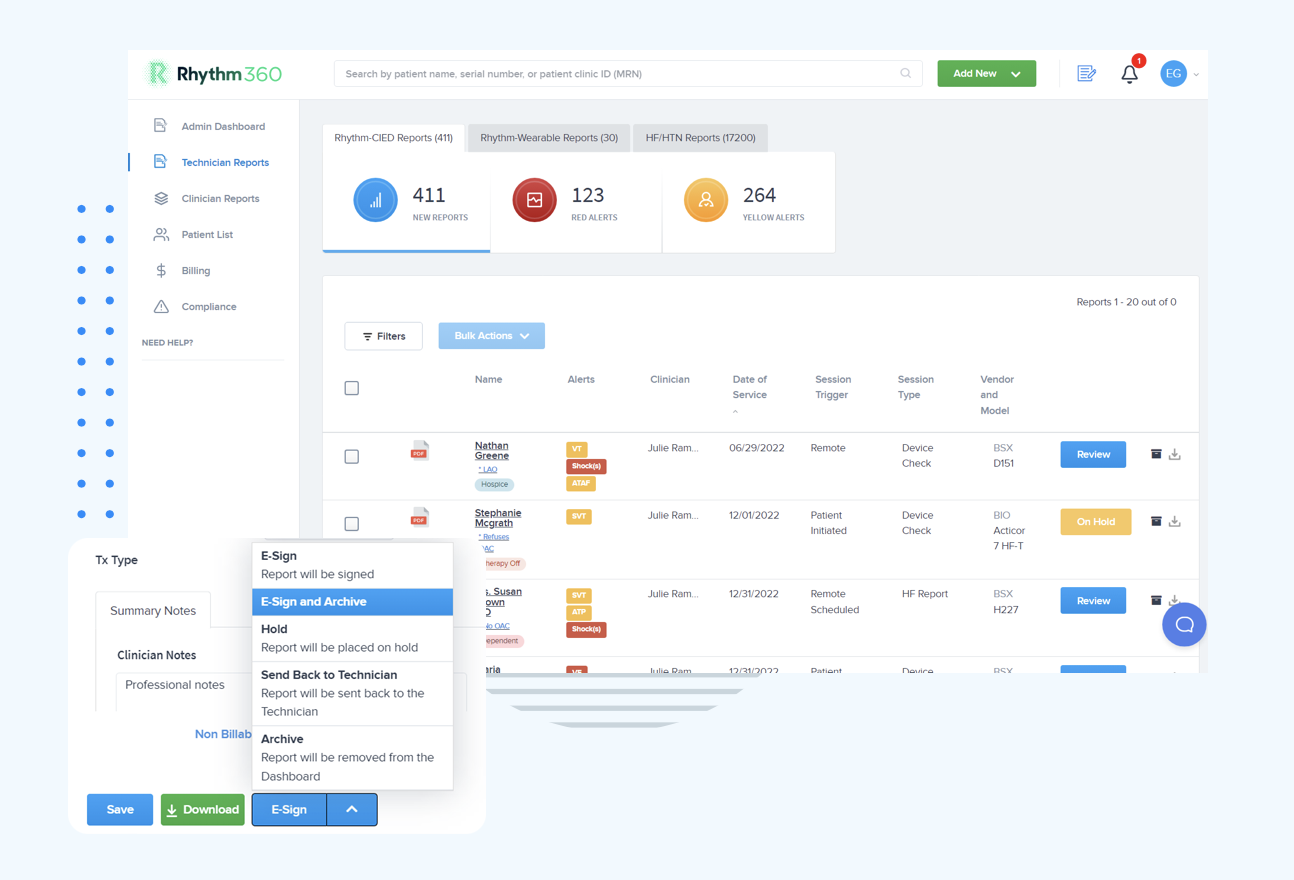
The vendor-neutral monitoring market includes several established platforms that support heart failure workflows. Understanding these differences helps clinics match solutions to their operational needs and growth plans. The comparison below focuses on three critical differentiators: breadth of device manufacturer support, AI triage effectiveness as reflected in response time reduction, and revenue improvement potential through billing automation.
| Platform | Vendor-Neutral Support | AI Triage Capability | Revenue Optimization |
|---|---|---|---|
| Rhythm360 | All OEMs supported | 80% response reduction | High uplift potential |
| PaceMate | Partial OEM coverage | Alert filtering available | Moderate billing support |
| Octagos | Multi-vendor support | AI-driven filtering | Good billing integration |
| Implicity | Limited OEM support | Strong AI algorithms | Basic billing features |
Rhythm360 stands out through complete vendor neutrality that supports data integration from all major device manufacturers without separate contracts or custom builds. The platform’s high uptime comes from redundant data feeds and AI-powered extrapolation that maintain continuity even when OEM servers experience outages.
Implementation timelines also differ across platforms. Rhythm360 uses a streamlined onboarding process with bi-directional EHR integration for Epic and Cerner. Clinics typically complete setup within days or weeks, while legacy solutions often require several months.
Successful platform implementation starts with a clear assessment of current workflows, data silos, and integration needs. Teams first inventory existing OEM portals, device populations, and EHR systems to establish baseline metrics for operations and clinical performance.
Phased rollout strategies reduce disruption and speed up value realization. Clinics often begin with high-volume device populations or patients who generate frequent alerts. This focus concentrates early benefits, lets staff experience smoother workflows quickly, and builds support for broader deployment.
ROI measurement covers several dimensions, including response time reduction, improved revenue capture, and fewer readmissions. Cardiac Solutions achieved a 50% reduction (7% vs. 15%) in 30-day hospital readmissions for cardiovascular patients using MD Revolution’s RevUp remote patient monitoring. Telemonitoring for heart failure patients has also been linked with lower readmission odds.
A practical scenario shows this impact clearly. Saturday morning detection of new-onset atrial fibrillation through AI-prioritized alerts allows immediate anticoagulation. That timely action can prevent stroke and avoid an emergency department visit. Real-time monitoring turns reactive care into preventive management in cases like this.
Explore implementation strategies with our team to see how Rhythm360 adapts to your clinic’s specific workflows and patient mix.
AI capabilities continue to advance, with AI tools now detecting early signs of heart failure at least five years before symptoms appear through pattern recognition. Next-generation wearables that connect to remote monitoring platforms can lower hospitalization risk by catching irregular rhythms earlier.
Redundant data feed architectures address reliability expectations as healthcare systems require very high uptime for critical monitoring. This infrastructure keeps patient surveillance active even when individual OEM systems undergo maintenance or experience outages.
Implementation risks include ongoing alert fatigue if AI triage is poorly tuned and continued revenue leakage when billing workflows stay manual. Rhythm360 reduces these risks through proven AI algorithms and automated CPT code capture that supports compliant documentation for all billable monitoring activities.
Real-time heart failure monitoring reduces readmissions by surfacing early signs of decompensation. Continuous tracking of weight trends, activity levels, and device-detected parameters such as thoracic impedance provides early warning. Clinicians can then adjust medications, change treatment plans, or schedule urgent visits before patients require emergency hospitalization. Clinical studies show meaningful readmission reductions when teams act on these early alerts.
Effective vendor-neutral platforms support data integration from all major device manufacturers, including Medtronic, Abbott, Boston Scientific, and Biotronik, without separate technical builds. Rhythm360 leads this category through comprehensive OEM support, AI-powered alert triage, and seamless EHR integration. Its high-reliability architecture and automated billing capabilities set it apart from competitors that provide only partial vendor coverage or limited workflow automation.
Remote pacemaker monitoring starts with automatic data transmission from implanted devices to OEM servers, usually nightly or during scheduled interrogations. Vendor-neutral platforms then ingest this data through API connections, normalize it across manufacturer formats, and apply AI algorithms to flag clinically significant events. Prioritized alerts reach clinicians through mobile notifications, while routine reports flow into EHR systems with automated billing documentation for the appropriate CPT codes.
AI alerts improve clinic efficiency by sharply reducing non-actionable notifications that drain clinician attention. These systems filter false alarms and elevate genuine clinical events, which supports much faster response times for critical situations while lowering overall alert volume. Clinical teams can then focus on patients who need immediate help instead of managing overwhelming notification streams from multiple monitoring systems.
CIED remote monitoring reliability depends on consistent data transmission, strong system uptime, and smooth integration with existing workflows. Rhythm360 maintains the reliability standards discussed earlier through dual-feed architecture and intelligent gap-filling algorithms, supported by computer vision for additional data redundancy. Its comprehensive vendor neutrality and proven ROI make it a strong choice for practices that need dependable, scalable monitoring.
Real-time heart failure management platforms now serve as core infrastructure for modern cardiovascular care. The combination of AI-powered alert triage, vendor-neutral data integration, and automated billing workflows directly addresses the operational challenges that limit both efficiency and outcomes. Transform your monitoring workflows today by scheduling a Rhythm360 demo that shows how unified, intelligent systems improve patient care while strengthening clinic profitability.


