Reducing manual review of cardiac device alerts improves clinical outcomes, staff efficiency, and revenue capture. Faster response times to critical alerts prevent strokes through timely atrial fibrillation detection and anticoagulation initiation. Streamlined workflows reclaim staff time, so device technicians and nurses can focus on patient care instead of repetitive administrative tasks. Better alert management also helps practices capture previously missed revenue through accurate CPT code documentation and stronger billing compliance.
The stakes of inaction remain significant. Recent consensus guidelines emphasize the critical importance of risk-stratified alert management to prevent adverse patient outcomes. Practices that ignore systematic alert reduction strategies face ongoing staff burnout, higher regulatory compliance risks, and revenue losses that can reach 300% of potential earnings.
Successful implementation starts with a clear technical and operational foundation. Practices need a multi-OEM device mix, active EHR access through Epic or Cerner, baseline alert volume tracking, and HIPAA-compliant infrastructure. Staff should document current manual review times and identify key stakeholders such as electrophysiologists, device technicians, and clinic administrators.
Rhythm360 onboarding typically takes days to weeks, not months. The platform supports bi-directional EHR integrations, automated data normalization from all major OEMs, and comprehensive staff training. This rapid deployment lets practices realize benefits quickly while maintaining uninterrupted patient care.
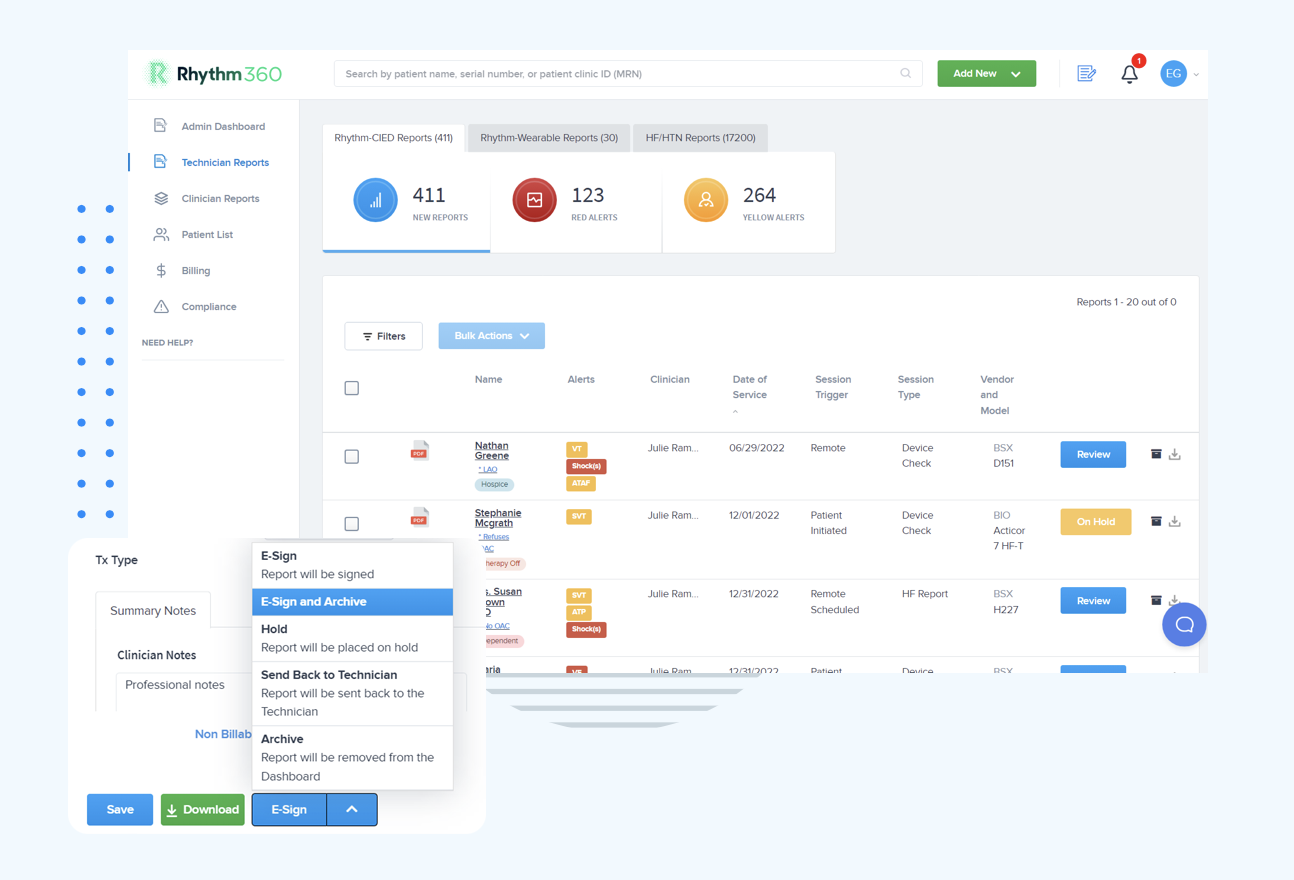
Step 1: Stratify Alerts by Clinical Urgency
Risk-based alert classification ensures the right team members see the right alerts at the right time. European Heart Rhythm Association guidelines recommend oral anticoagulation for device-detected atrial fibrillation burden exceeding 5.5 hours in one day in patients with CHA2DS2-VASc score ≥2. Create three priority levels to match this evidence: urgent for immediate response, moderate for 24-hour review, and routine for weekly assessment. This structure keeps critical events from getting buried in low-value noise.
| Alert Type | Threshold | Priority Level | Response Time |
|---|---|---|---|
| Atrial Fibrillation | >5.5 hours in one day (high-risk patients) | Urgent | Immediate |
| Ventricular Tachycardia | Elevated rates | Urgent | Immediate |
| Device Malfunction | Lead impedance anomalies | Moderate | 24 hours |
| Battery Status | ERI/RRT | Moderate | 24 hours |
Step 2: Use the Rule of 3 for Cardiac Alerts
The Rule of 3 methodology filters repetitive, non-actionable notifications before they reach clinicians. This evidence-based approach requires three consecutive similar alerts within a defined time window before triggering clinical review. The rule reduces noise from transient events, device self-corrections, and patient activity-related fluctuations. At the same time, it preserves meaningful patterns that signal real clinical risk.
Step 3: Add AI Triage for CIED Alerts
AI triage systems such as Rhythm360’s algorithms automatically prioritize alerts based on clinical significance. These AI-powered platforms use redundant feeds and computer vision technology to maintain high reliability, so critical events are not missed due to technical failures. The models learn from historical patterns, which steadily improves accuracy and reduces false positives over time.
Step 4: Consolidate Alerts with Vendor-Neutral RPM Platforms
Vendor-neutral remote patient monitoring platforms eliminate the need to log into multiple OEM portals. Rhythm360 consolidates data from Medtronic, Abbott, Boston Scientific, and Biotronik into a single dashboard with EHR integration. This consolidation removes portal-hopping, cuts data entry errors, and gives teams a complete view of each patient across all device types. Schedule a Rhythm360 demo to see multi-OEM integration and streamlined workflows in action.
Step 5: Automate Remote Monitoring Alert Workflows
Automated workflows route alerts to the right clinical staff based on urgency and expertise. Configure mobile notifications for urgent events, automated report generation for routine checks, and clear escalation paths for missed responses. HIPAA-compliant mobile access lets clinicians review transmissions and coordinate care from any location. This access reduces on-call burden and shortens response times.
Step 6: Educate Teams and Run Ongoing Audits
Team education anchors every alert reduction strategy. Train all staff members on new alert management protocols, including device technicians, nurses, and physicians. Once trained, these team members need standardized checklists for alert review, patient communication, and documentation requirements to keep execution consistent. Regular audits then verify adherence to protocols and highlight opportunities for continuous improvement.
Step 7: Measure ROI and Expand the Program
Clear metrics prove impact and guide scaling decisions. Track key performance indicators such as alert response times, staff productivity, and revenue capture through accurate CPT code billing. Monitor patient outcomes, staff satisfaction, and operational efficiency gains to round out the picture. Use these metrics to demonstrate return on investment and decide when to extend the program to additional service lines or patient populations.
| Metric | Before Implementation | After Rhythm360 | Improvement |
|---|---|---|---|
| Alert Response Time | 24 hours | under 5 hours | 80% reduction |
| Manual Review Hours | 40 hours/week | significantly reduced | 80% reduction |
| Revenue Capture | Baseline | aligned with 300% uplift cited earlier | 3x improvement |
| Staff Satisfaction | 65% | improved | notable increase |
Real-world implementations show consistent gains across clinical and operational metrics. Practices using comprehensive alert reduction strategies report 80% faster response times to critical events, with average response dropping from 24 hours to under 5 hours. AI-powered noise filtering cuts non-actionable alerts, so clinical staff can focus on patients who truly need intervention.
Revenue improvements match these clinical gains. Practices capture the 300% revenue uplift mentioned earlier through stronger CPT code documentation and more efficient workflows. Rhythm360’s dashboard gives real-time visibility into patient compliance, critical alerts, and revenue opportunities, which supports data-driven decisions and ongoing refinement.
Alert reduction strategies must fit the size and structure of each organization. Solo practitioners benefit from simplified workflows, automated reporting, and clear daily priorities. Large health systems require more complex routing rules, shared protocols, and coordination across multiple departments. Rhythm360’s flexible architecture supports both settings through customizable alert thresholds and scalable user management.
Many practices move next into broader remote monitoring and chronic disease management. Programs can expand beyond CIED monitoring to heart failure and hypertension populations. Integration with technologies such as CardioMEMS pulmonary artery monitors and continuous glucose monitoring adds new revenue streams. These integrations also support earlier intervention and better long-term outcomes.
The Rule of 3 is an evidence-based alert filtering method that requires three consecutive similar alerts within a defined time window before clinical review. This structure reduces non-actionable notifications from transient events, device self-corrections, and patient activity fluctuations. At the same time, it preserves clinically significant patterns that signal a need for intervention.
Rhythm360 delivers comprehensive vendor-neutral integration across all major OEMs, while PaceMate acquired the PaceArt Optima system from Medtronic. Rhythm360’s AI-powered triage system uses redundant feeds and computer vision technology to provide strong reliability and clinical decision support. These capabilities go beyond traditional database systems that focus mainly on data storage.
Rhythm360 implementation usually takes days to weeks. The process includes EHR integration setup, staff training, alert threshold configuration, and workflow design. Most practices see measurable improvements in alert management within the first month, with full refinement typically achieved within 90 days.
Rhythm360 uses a SaaS-based pricing model that scales with clinic size and platform usage. This structure offers flexible investment options without high upfront setup fees. The return on investment often exceeds 300% through improved billing capture, staff efficiency gains, and lower operational overhead, which makes the platform cost-neutral or revenue-positive for most practices.
Recent consensus guidelines emphasize risk-stratified alert management and timely response protocols for critical events. Practices must use systematic approaches to alert triage, documentation, and patient communication to stay compliant with evolving standards. Rhythm360’s platform incorporates these requirements through configurable workflows and detailed audit trails.
The seven-step approach to reducing manual review of cardiac device alerts by 80% gives practices a practical roadmap for change. Success shows up as faster response times, lower staff burnout, better patient outcomes, and substantial revenue increases through stronger billing practices. The combination of AI-powered triage, vendor-neutral consolidation, and automated workflows creates durable improvements for patients, providers, and practice profitability. Schedule your Rhythm360 demo today to start applying these strategies and see measurable results within weeks.


